- Addiction Treatment
- After Care Programs
- Get loved one into rehab
- Holistic Treatment
- Interventions
- Life After Addiction Treatment
- Outpatient Drug Rehab
- Sober Living Homes
- Addiction Recovery Tips
- What Are Opiates
- Helping Loved One with a Drug Addiction
- 5 Ways To Recover From Drug-Addiction
- Warning Signs Of Pain Killer Addiction
- Buprenorphine
- Drug Addiction
- Pain Killer Abuse
- Opiate Addiction
- 5-Symptoms-Of-Prescription-Drug-Addiction
- Opiate Addiction Statistics
- Opioid Dependence
- Prescription Drug Abuse Statistics
- Warning Signs Of Prescription Drug Addiction
- Oxycontin Addiction
- Pain Killer Addiction
- Percocet Addiction
- Prescription Drug Addiction
- Hydrocodone Addiction
- Morphine Addiction
- Effects of Drug Addiction
- Signs & Symptoms of Drug Addiction
- Drug Addiction Treatment Act
- Vicodin Addiction
- Drug Detox
- What Is Drug Detox
- Codeine Detox
- Heroin Detox
- Opiate Detox
- Lorcet Detox
- Inpatient drug detox
- Fentanyl Detox
- Medical Drug Detox
- Oxycodone Detox
- Oxycontin Withdrawal What To Expect
- Morphine Detox
- Morphine Withdrawal
- Vicodin Detox
- Painkiller Withdrawal
- Percocet Detox
- Rapid Opiate Detox
- Opiate Withdrawal
- Prescription Drug Detox
- Drug Treatment
- Doctor’s Note
- About Us
- Suboxone FAQ
- How do you get a prescription for buprenorphine?
- How much does Suboxone cost?
- How to Find Suboxone Doctor Near me?
- What are the stages of change in recovery for addiction?
- What happens when you come out of rehab?
- What happens after drug and alcohol rehab?
- How Long Will It Take to Complete Suboxone Treatment?
- What Is the Best Time of Day to Take Suboxone?
- How to Get Prescribed Suboxone for Free?
- What is an adverse reaction for Suboxone?
- How to Get Suboxone Without Insurance
- Difference Between SUBOXONE® and Buprenorphine?
- Are You Sober on Suboxone? Yes & Here Is Why
- Is Suboxone used to treat depression?
- What is the most common method of payment for buprenorphine treatment?
- What are the special precautions of buprenorphine?
- What Is The Death Rate Of Buprenorphine?
- Can I prescribe buprenorphine for chronic pain?
- What is Opioid Therapy Used For?
- What is the best treatment for opioid use disorder?
- What are the special precautions of buprenorphine?
- How to Get Suboxone Without Insurance
- What is the most common method of payment for buprenorphine treatment?
- Are You Sober on Suboxone? Yes & Here Is Why
- What Happens If I Miss A Day/Dose Of Suboxone?
- What Are Suboxone Withdrawal Symptoms?
- Can Suboxone Be Used to Treat Drug & Alcohol Addiction?
- What drugs are classified as opioids?
- Insurance Coverage for Medication-Assisted Treatment (MAT)
- Contact Us
What is Buprenorphine?
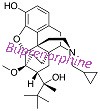
Buprenorphine is an FDA approved opioid addiction treatment. Currently Subutex® & Suboxone® are the only Buprenorphine medications approved by the FDA.
Buprenorphine itself is opioid itself, but the maximal effects are less than other more dangerous opioid agonist like methadone and herion. By producing enough agonist, individuals taking Buprenophine that have become addicted to other opioids are able to discontinue abuse with minimized withdrawl side-effects.
In 1965, K.W. Bentley discovered the class of compounds synthesized from an alkaloid of thebaine, the opium poppy plant, known as Papaver somniferum. Among these semi-synthetic compounds is Buprenorphine – the first in a series of opioid agonists. Many were more than 1000 times more effective than the analgesic, morphine.
In the 1980s, Reckitt & Colman, today known as Reckitt Benckiser, introduced Buprenorphine hydrochloride for sale. Buprenorphine, an analgesic, was first made in sublingual tablets of 0.2 mg (Temgesic). It was also made as an injectable of 0.3 mg/ml (Buprenex).
Advertisement
Buprenorphine Successfully Treats Opioid Addiction
Opioids are narcotics used in pain management and to induce sleep.
Physiologic reactions, similar to those caused by a substance found in nature, are produced by a drug known as an opioid agonist, that merges with a cell’s opioid receptor. Opiate receptors are scattered abundantly throughout the digestive tract, spinal cord and the brain. Morphine is an opioid agonist.
On the other hand, a drug known as an opioid antagonist will combine with and block nerve receptors, thwarting the physiological actions of a substance found in nature. Thus, it may reverse and even block the actions of an opioid agonist. Naloxone is a typical opioid antagonist.
Buprenorphine is a partial agonist opioid; It can generate the usual opioid agonist effects but, not as greatly as those produced by full agonists, such as heroin and methadone. Full agonist opioids have the risk of side effects, abuse, and addiction. Not only does Buprenorphine have fewer risks, but it can negate all the effects of opioid agonists, and even lessen withdrawal symptoms in an addict whose bloodstream is currently carrying a full agonist.
Low doses of Buprenorphine enable patients to stop misusing drugs without suffering intense withdrawal symptoms. A “ceiling effect” is reached when the agonist effects no longer increase in concurrence with dosage and stops at a moderate dose. A Buprenorphine overdose is less likely than an overdose of a full opioid agonist.
Laws, Limitation, and Lack of treatment
Although Buprenorphine promised great results, due to outdated guidelines, it was unavailable to most addicts; Doctors were limited to treating only thirty addict patients at any given time, and only in specific addiction treatment centers. The numbers of addicts seeking medical help had been sharply increasing and countless addicts had died for lack of medical treatment needed to overcome their addiction. A cacophony of concerns was heard in both the medical community and in buprenorphine treatment centers. The few addicts successfully treated with Buprenorphine brought about changes in the laws that enabled even greater numbers of addicts to also successfully beat their habit.
Advertisement
DATA 2000
The Drug Addiction Treatment Act (DATA) went into effect in the year of 2000. Qualified physicians may now prescribe narcotics that are specifically approved for use in settings other than methadone clinics.
DATA 2000 also decreases the regulations that burden physicians and allows them to attain waivers described in the Controlled Substances Act (CSA). The qualifying credentials of the physician must be noted in the Intent Notification. Other papers validating the physician’s capacity to send in-therapy addiction patients to non-pharmacologic therapy must be included. The physician must also note that, regardless of the number of office-based practices the physician may have, a limit of 30 or fewer patients will be in addiction therapy and counseling during the first year.
One year from the date of the primary Letter of Intent, the physician can present a second notice stating necessity and intention of treating up to, but not more than 100 patients.
Detoxification, Medically Assisted Withdrawl
Jacqueline H. Kostick, PhamD in the article “Buprenorphine Offers Alternative to Methadone for Opioid Dependence”, observes that Methadone has its limitations in the treatment of opioid dependency. Since it is classified as a controlled substance, Methadone must be used only in hospitals or at a Methadone addiction clinic.
Buprenorphine, as a Methadone replacement in the treatment of opioid dependency, was found to be just as effective. Because Buprenorphine, as a partial agonistic opioid, contains properties that aid in the prevention of drug abuse, it has become the chosen drug in treating addicts during the maintenance period.
Buprenorphine’s sublingual tablet formulations, Suboxone and Subutex, was approved by the (FDA) Food and Drug Administration in October 2002, for detoxifying and for the longtime therapy substitute for methadone in the treatment and therapy of opioid dependency. Buprenorphine currently predominates as the drug of choice to aid patients while they are in heroin and opium withdrawal.
Advertisement
Side Effects of Buprenorphine
Like other opioids, Buprenorphine can have withdrawl side effects:
- Unable to Sleep
- Cramps & Muscle Aching
- Diarrhea, Nausea, & Vomiting
- Cravings
- Fever
- Irritability
Addiction Therapy
There are 3 phases of Buprenorphine treatment therapy
- Induction Phase – 12 to 24 hours after last opioid use, where Buprenorphine is medically administered.
- Stabilization Phase – patient no longer craves opioid, useage has stopped or decreased significantly, and no longer experiencing side effects.
- Maintenance Phase – the detox phase where patient usage of opioid has stopped and Buprenorphine dosage is steady or ended completely.
Sources:
http://buprenorphine.samhsa.gov/about.html
http://www.merriam-webster.com/dictionary/opiate?show=0&t=1310002209
http://buprenorphine.samhsa.gov/fulllaw.html
http://www.medscape.com/viewarticle/553558
Articles
How to find Online Suboxone Doctors that Accept MedicaidLocating a Skilled Suboxone Doctor Near You: A Comprehensive GuideUnveiling the Grip of OxyContin: A Comprehensive Guide to Overcoming AddictionNavigating Addiction Recovery with Buprenorphine TreatmentDual Diagnosis: Addressing Co-Occurring Mental Health Disorders in Substance Abuse Treatment
